Around three per cent (6,100) of the 200,000 residents in Australia’s aged care facilities had COVID, as of July 22, in addition to 3,400 staff. About 1,000 facilities – nearly 40 per cent of the total – had an outbreak.

Aged care residents are also disproportionately dying of COVID. Those in nursing homes account for nearly 30 per cent of the 11,000 deaths from COVID in Australia throughout the pandemic.
Why is this happening?
Age is a major risk factor for COVID. People aged 70 and over make up 85 per cent of all reported COVID deaths.
People in residential care are the most frail and at risk. Aged care residents make up around 40 per cent of the deaths of older Australians, but only about five per cent of the population aged 65 and over live in residential care.
We’ve long known how to reduce the spread of COVID and unnecessary deaths. Effective responses throughout the aged care sector include:
- all residents and staff being fully vaccinated
- appropriate availability of personal protective equipment and rapid antigen tests (RATs)
- mask mandates for staff and visitors
- widespread use of antiviral treatments for those who catch COVID
- rapid responses to outbreaks, including a surge workforce and coordination with home care, GPs and hospital services.
But while mask mandates remain a requirement in residential aged care for staff and visitors, and RATS and PPE are now generally available, the other responses are still patchy, piecemeal and poorly coordinated.
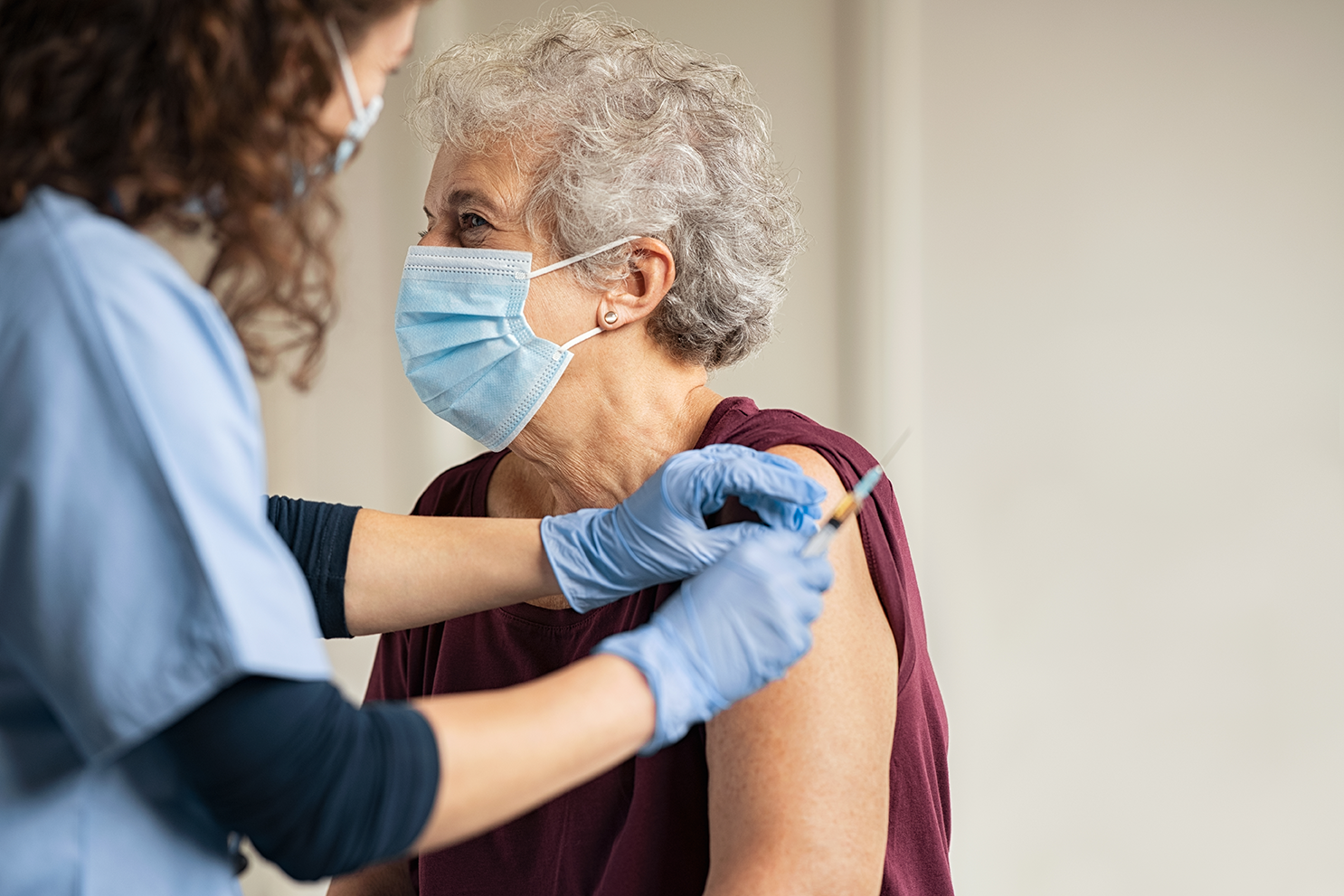
Vaccination
Vaccination is the most important protection against COVID. People who are unvaccinated are about 50 times more likely to die from COVID compared with those who are fully vaccinated.
Yet, vaccinations in residential aged care has been a shambles. Early on in the rollout for aged care, staff weren’t fully vaccinated, there were squabbles over staff vaccination mandates, vaccination data was unavailable, and it was unclear who was responsible for making sure vaccination occurred.
While mandates have lifted worker vaccination rates, in June this year, only 50 per cent of aged care residents were fully boosted with fourth doses.
That has improved following pressure from the new government. But even now, a quarter of residents are still not fully vaccinated with recommended boosters.
More needs to be done to systematically follow up facilities with low vaccination rates.

Antivirals
Early use of antivirals significantly reduces the risk of hospitalisation and death from COVID, possibly as much as 80 per cent.
It has been clear for about six months that antivirals are a safe and effective COVID treatment. However, it wasn’t until July 11 that the Commonwealth Chief Medical Officer advised that all Australians 70 or older should be offered antiviral treatment within 24 hours when they test positive for COVID (where clinically appropriate).
The reality is that many older people who could benefit from antivirals aren’t getting them and they are going to waste, with thousands of doses nearing their use-by dates.
Rapid responses to out outbreaks
The new federal government appears to be tackling the issue with new urgency. The new aged care minister, Anika Wells, has released a “winter plan” to try to address the aged care crisis.
The plan includes prevention, outbreak management and recovery. But the plan continues to put most of the responsibility of prevention and management on individual providers – a strategy that has been ineffective in the past.
The federal government has almost no capacity to effectively coordinate a winter response across residential care, home care and health and support services within local service networks where it is needed.
Ideally, this would see close working relationships between aged care facilities, GPs and local hospitals, including the redeployment of clinical and support staff across facilities as required. This happened in Victoria during the 2020 outbreak.
But despite the recent Royal Commission’s recommendation to do so, the federal government has not put in place local or regional bodies or authorities to plan, coordinate and manage aged care.
Staff shortages
These pressures are hugely exacerbated by staff shortages. The over-reliance on a privatised market model for aged care and the decades-long under-investment in training, supervision, pay and conditions for aged care workers has come home to roost at the worst possible time.
Estimates suggest there is a shortfall of 35,000 workers in aged care, double the problem last year.
The industry is hoping the work value case before the Fair Work Commission will make a difference on these issues. Personal care workers in aged care are paid about the same as workers at McDonald’s – in some cases, less. Unions are arguing for a 25 per cent increase in pay, which should make aged care a more desirable job, but this case won’t be determined for months.
In the meantime, the industry still does not have a realistic workforce strategy. The federal government is scrambling to implement short-term measures through a “surge workforce”, including the recent deployment of 200 military personnel.
But this is unlikely to be enough to address the staff shortages associated with the winter wave. Some providers are now reporting they are down 20 to 40 per cent of staff.
The result is excess hospitalisation and death, misery for residents and their families, and stress for staff and providers. If the situation continues to deteriorate, this will have to become a major priority for National Cabinet.
And the already stretched state health systems will have to play a greater role to fix the immediate problems.
Author: Hal Swerissen, Emeritus Professor, La Trobe University
This article is republished from The Conversation under a Creative Commons license. Read the original article.